New connected devices could help doctors prescribe anti-coagulant medication for just the right amount of time.
Researchers in France are developing a new smart, connected stent containing sensors that can non-invasively monitor how an artery heals after stent implantation. The sensors can analyze whether the stent is becoming covered with too many smooth muscle cells, which can lead to potentially fatal restenosis, or if blood clots are forming on the device, which can lead to a fresh heart attack. The sensors will wirelessly transmit their data to the outside world so that it can be consulted by both patients and their doctors.
The two leading cardiovascular killers today are coronary heart disease and stroke. Both occur when endothelial cells, which line the artery wall, start to chronically dysfunction. The arterial wall thickens (known as arthrosclerosis) and the artery itself may eventually become blocked entirely.
Coronary stents are the main way of treating this problem. These mesh-like scaffolds, usually made of metal, are threaded into blocked arteries and the structures are then expanded, generally by inflating a balloon inside the stent, to hold the vessel open.
Stent can help observe endothelial damage. The animation shows how the stent is inserted into an artery and the arterial wall with its endothelial cells can be clearly seen.Credit: Courtesy of A.Barakat
ANTI-COAGULANTS, YES, BUT FOR HOW LONG?
The problem is that when a stent is placed in an artery, it damages the arterial wall (and in particular, completely obliterates the endothelial layer). One of the consequences is that blood coagulates on the surface of the stent. Clots formed during this process can lead to the opposite of what is intended – that is, a new heart attack or stroke.
To overcome this problem, patients are given anti-coagulants but it is difficult to know how long to prescribe this medication. Some patients heal within a matter of weeks, while others (especially very old patients) can take years to do so. And worryingly, during treatment, the patient cannot undergo any other surgical or dental procedure.
ENTER CONNECTED STENTS
“The connected stents could come into their own here,” explains Abdul Barakat, professor at the Ecole Polytechnique in Palaiseau near Paris and holder of the AXA Chair for Cardiovascular Engineering, who is helping to develop the devices in collaboration with Instent, a start-up created in 2014 with his former PhD student Franz Bozsak. “The stents contain electronic sensors that can send information as to how quickly the artery is healing, so a doctor can stop the anti-coagulants at the right time.”

Professor Abdul Barakat.Credit: Courtesy of A.Barakat
The sensors, which can be made from metals or other materials, are powered by induction (think of your bus or train pass, which works by swiping it across a magnetic support) and are placed on the different struts on the stent, which are roughly 80 μm thick. They measure around 50 μm x 50 μm x 10 μm and are embedded in a biocompatible 10 μm-thick film.
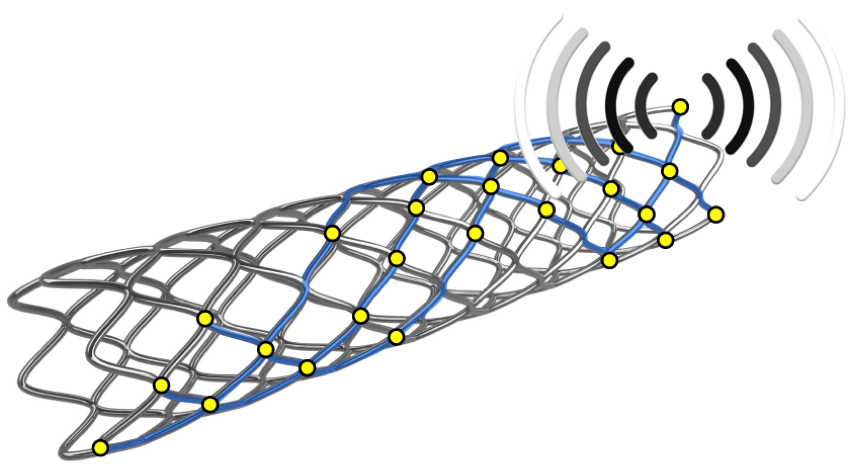
An image of the smart connected stent.Credit: Courtesy of A.Barakat
SENDING THE APPROPRIATE SIGNAL
When covered with arterial tissue, the sensors can distinguish between three different possible scenarios and send the appropriate signal. The first, as mentioned above, is thrombosis, or blood clotting. The second is normal arterial wall healing, which is characterized by the stent being covered with new endothelial cells. The third is restenosis, or the uncontrolled proliferation of smooth muscle cells on the stent that can re-block the artery.
“The key thing for us is to be able to establish whether the sensors are covered with endothelial cells, smooth muscle cells, a blood clot or nothing,” says Barakat. “In vitroexperiments, and preliminary in vivo testing in pigs, indeed show that different signals are sent depending on the type of situation present and that the signals are sufficiently different to be distinguished.”
TOWARDS A BETTER STENT DESIGN
Beyond continuous stent follow-up, the data produced by the sensors will also be important for understanding which stent types and designs work best for particular patients, he adds. “This ‘big data/machine learning’ aspect of our work will help us to move towards a patient-specific approach to stenting – something that is lacking right now. Ultimately, we may even be able to design better stents and move away from designs that cause the most problems.
Instent now has seven employees and its mission is to get these smart connected devices to the patient, ideally by integrating the biocompatible film that goes on the stent and the associated wireless communication system with existing stents of large manufacturers. We hope to have a fully operational prototype by the end of this year and the first clinical trials in humans could start in 2018. If all goes to plan, patients could see the first connected stents by the end of this decade.”
The approach is so promising that Ulrich Sigwart, one of the first physicians to have implanted stents into patients and who is now honorary professor at the University of Geneva in Switzerland, has decided to invest in the new project himself. "Stents have fundamentally changed the way that patients with coronary heart disease and other arterial diseases can be treated without major surgery,” he says. “Up to now, there was only one way of finding out how the body had accepted the implant, and this was in an invasive way. What is more, the duration of drug treatment to inhibit thrombosis was vaguely defined. I find the concept of monitoring proper endothelialization of stents from the outside most attractive as it allows us to keep an eye on such implants so that we can make clinical decision without bothering the patient."
Deploying the sensor on the stent. The stent wire, monitoring system and drug layer can be clearly seen in the blow-up.Courtesy of A.Barakat
A CONNECTED FUTURE
The new stents follow the trend for connected medical devices in general, and we need to prepare ourselves in the best way possible for this new era, says Barakat. There is huge promise, but we need to be conscientious and responsible. Patient privacy is crucial and the data from these technologies will need to be protected.
Source : Scientific American
Discover research projects related to the topic
Mental Health & Neurology
AXA Chair
Belgium
Neuropsychiatric Diseases and Basal Ganglia: Underlying Mechanisms
A central hub in the brain, the basal ganglia governs a diverse array of functions including voluntary movement, procedural memory, habit... Read more

Alban
DE KERCHOVE D'EXAERDE
Université libre de Bruxelles
Women's Health
AXA Chair
Spain
Understanding Menopause's Effect on Women's Cardiovascular Risk
Cardiovascular disease (CVD) is the leading cause of mortality for women worldwide, yet women remain understudied. Atherosclerosis, the main pathology underlying... Read more
.thumbnail.jpg)
Inés
PINEDA-TORRA

